Welcome to our comprehensive guide on understanding cholesterol-like plaque buildup, a common cardiovascular health concern. Cholesterol plaques, also referred to as arterial plaque, can lead to arterial blockage, increasing the risk of heart attack and stroke. It is crucial to grasp the factors contributing to plaque formation and learn how to prevent and manage this condition for optimal heart health.
Key Takeaways:
- Cholesterol plaques can cause heart diseases like coronary artery disease and peripheral arterial disease.
- Plaque formation occurs when bad cholesterol (LDL) damages artery walls and accumulates over time.
- Risk factors for plaque formation include high cholesterol, genetics, smoking, obesity, and sedentary lifestyle.
- Plaque buildup can lead to complications such as angina, shortness of breath, and cardiovascular events like heart attack and stroke.
- Lifestyle changes, including a healthy diet, regular exercise, and smoking cessation, can help prevent plaque formation.
Causes and Risk Factors of Plaque Formation
Plaque formation, characterized by the accumulation of cholesterol-like plaque in the arterial walls, is primarily caused by high cholesterol levels. However, several risk factors contribute to the development of plaque and increase the likelihood of atherosclerosis.
- A diet high in saturated and trans fats is one of the leading culprits for high cholesterol and plaque formation. Consuming foods such as red meat, full-fat dairy products, fried foods, and processed snacks can elevate cholesterol levels.
- Genetics: Your family history plays a role in determining your cholesterol levels and susceptibility to plaque formation. If you have close relatives with a history of high cholesterol or cardiovascular disease, you may be more prone to developing plaque.
- As you age, the risk of plaque formation increases. Over time, cholesterol levels can gradually rise, making it essential to monitor and manage your cholesterol levels through routine check-ups.
- Smoking: Tobacco smoke contains harmful chemicals that damage blood vessels, impair their function, and contribute to the development of plaque. Smoking not only increases the risk of plaque formation but also accelerates its progression.
- Conditions such as high blood pressure and diabetes can lead to endothelial dysfunction, making arteries more susceptible to plaque buildup.
- Obesity and a sedentary lifestyle can negatively impact cholesterol levels and contribute to plaque formation. Regular physical activity and weight management are essential for reducing the risk of plaque buildup.
- Prolonged stress and high-stress levels can have detrimental effects on your cardiovascular health. Stress management techniques, such as meditation, exercise, and counseling, can help mitigate the risk of plaque formation.
An Overview of Risk Factors for Plaque Formation
| Risk Factor | Description |
|---|---|
| High Cholesterol Diet | A diet rich in saturated and trans fats increases cholesterol levels and contributes to plaque formation. |
| Genetics | Your family history can determine your susceptibility to high cholesterol and plaque buildup. |
| Age | As you get older, the risk of plaque formation and atherosclerosis increases. |
| Smoking | Tobacco smoke damages blood vessels and accelerates plaque buildup. |
| High Blood Pressure | Elevated blood pressure can lead to endothelial dysfunction and plaque formation. |
| Diabetes | Unmanaged diabetes can contribute to plaque formation and atherosclerosis. |
| Obesity and Sedentary Lifestyle | Lack of physical activity and excess weight increase the risk of high cholesterol and plaque formation. |
| Stress | Chronic stress can negatively impact cardiovascular health and contribute to plaque buildup. |
To reduce the risk of plaque formation and atherosclerosis, it’s crucial to make lifestyle changes that promote heart health. Adopting a balanced diet low in saturated fats, engaging in regular physical exercise, quitting smoking, and managing stress levels are effective strategies to minimize plaque accumulation. By addressing these risk factors and taking proactive steps towards a healthy lifestyle, you can significantly lower your risk of developing plaque buildup and its associated cardiovascular complications.
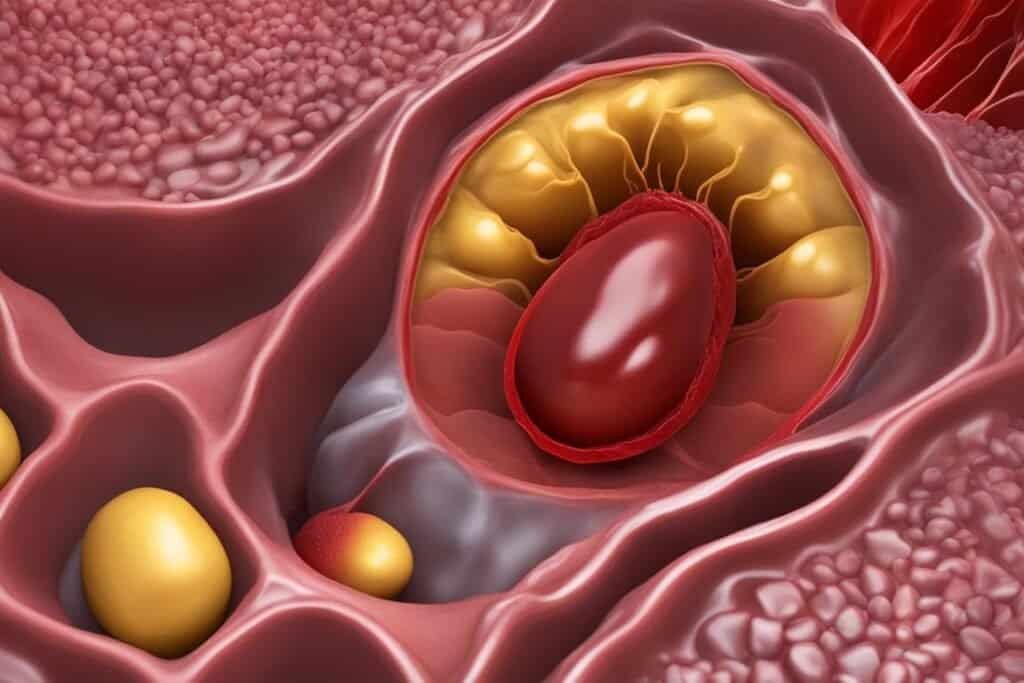
Complications and Symptoms of Plaque Buildup
If plaque buildup becomes severe, it can lead to various complications and health issues. These include:
- Coronary Artery Disease: Plaque buildup in the coronary arteries can restrict blood flow to the heart, leading to chest pain known as angina.
- Peripheral Arterial Disease: Plaque buildup in the peripheral arteries, typically in the legs and feet, can cause pain, numbness, and poor circulation.
- Carotid Artery Disease: Plaque in the carotid arteries, which supply blood to the brain, can increase the risk of stroke.
- Heart Attack: A heart attack, also known as a myocardial infarction, can occur if a plaque ruptures, causing a blood clot that blocks blood flow to the heart.
- Stroke: Plaque in the arteries that supply blood to the brain can lead to a stroke when blood flow is blocked or reduced.
These conditions can cause a range of symptoms, including:
- Chest pain (angina) that may radiate to the arm, shoulder, jaw, or back
- Shortness of breath, especially during physical activity
- Heart palpitations or irregular heartbeat
- Dizziness or lightheadedness
- Weakness and fatigue
- Slurred speech or difficulty speaking
- Facial drooping or weakness on one side of the face
- Numbness or weakness on one side of the body
- Vision changes or sudden vision loss
It’s important to note that in many cases, plaque buildup may not cause any noticeable symptoms until a cardiovascular event, such as a heart attack or stroke, occurs. Regular monitoring of cardiovascular health and maintaining a healthy lifestyle are crucial for early detection and prevention.
Diagnosing and Monitoring Plaque Buildup
Plaque buildup in the arteries can have serious implications for cardiovascular health. In order to effectively diagnose and monitor plaque buildup, cholesterol testing is essential. Specifically, a lipid panel is used to assess various aspects of cholesterol levels and provide crucial insights into the presence and severity of plaque formation.
A lipid panel measures key parameters, including:
- Total cholesterol
- HDL (good cholesterol)
- LDL (bad cholesterol)
- Triglycerides
- Non-HDL cholesterol
- The ratio between total cholesterol and HDL
By analyzing these measurements, healthcare professionals can evaluate an individual’s cholesterol profile and assess the risk of plaque buildup. Regular cholesterol testing is particularly important for those with known risk factors for cardiovascular disease.
Monitoring cholesterol levels through consistent testing enables early detection of any adverse changes in lipid profiles. By identifying high LDL cholesterol levels or imbalances in the lipid panel, appropriate interventions can be implemented to prevent the progression of plaque buildup and the associated risks.
Possible Results of a Lipid Panel
| Cholesterol Parameter | Desirable Level | Slightly Borderline | High Risk |
|---|---|---|---|
| Total Cholesterol | <200 mg/dL | 200-239 mg/dL | >240 mg/dL |
| HDL (Good Cholesterol) | >60 mg/dL | 40-59 mg/dL | <40 mg/dL |
| LDL (Bad Cholesterol) | <100 mg/dL | 100-129 mg/dL | >130 mg/dL |
| Triglycerides | <150 mg/dL | 150-199 mg/dL | >200 mg/dL |
| Non-HDL Cholesterol | <130 mg/dL | 130-159 mg/dL | >160 mg/dL |
| Total Cholesterol to HDL Ratio | <4.5 | 4.5-5.0 | >5.0 |
The above table illustrates the desirable, slightly borderline, and high-risk levels for each cholesterol parameter. By comparing individual test results to these reference ranges, healthcare professionals can gain a comprehensive understanding of an individual’s cholesterol profile and make informed decisions on appropriate treatment plans.
Remember, regular cholesterol testing is crucial to effectively diagnose and monitor plaque buildup. Consult with your healthcare provider to determine the appropriate frequency of cholesterol testing based on your individual health status and risk factors.
Treatment and Management of Plaque Buildup
If you have been diagnosed with plaque buildup and high cholesterol levels, don’t worry! There are effective treatments and management strategies available to help you reduce plaque, lower cholesterol, and improve your cardiovascular health. The key is to combine lifestyle changes with appropriate cholesterol medications prescribed by your healthcare provider.
Lifestyle Changes for Cholesterol Management
To support your cholesterol management and reduce plaque buildup, consider making the following lifestyle changes:
- Adopt a heart-healthy diet: Focus on consuming foods low in saturated fats, trans fats, and cholesterol. Include plenty of fruits, vegetables, whole grains, and lean proteins in your meals.
- Engage in regular exercise: Aim for at least 150 minutes of moderate-intensity aerobic activity or 75 minutes of vigorous-intensity aerobic activity every week. Additionally, incorporate strength training exercises two or more days per week.
- Maintain a healthy weight: Losing excess weight can help lower LDL cholesterol levels and reduce the strain on your cardiovascular system.
- Quit smoking: Smoking damages your blood vessels and raises your risk of plaque buildup. Quitting smoking is one of the most important steps you can take to improve your heart health.
- Manage stress: Find healthy ways to cope with stress, such as practicing relaxation techniques, engaging in hobbies, or seeking support from loved ones.
Cholesterol Medications
In addition to lifestyle changes, your healthcare provider may recommend cholesterol-lowering medications to further manage plaque buildup and cholesterol levels. Commonly prescribed medications for plaque reduction include:
- Statins: These medications are highly effective in lowering LDL cholesterol levels and reducing the risk of cardiovascular events. They work by inhibiting an enzyme involved in cholesterol production in the liver.
- Fibrates: Fibrates primarily target high triglyceride levels and can also help increase HDL cholesterol levels.
- Niacin: Niacin, or vitamin B3, can lower LDL cholesterol and triglyceride levels while increasing HDL cholesterol.
- Bile Acid Sequestrants: These medications bind to bile acids in the intestines, preventing their reabsorption and ultimately reducing LDL cholesterol.
- Ezetimibe: Ezetimibe works by blocking the absorption of cholesterol in the small intestine, leading to lower LDL levels.
- Plant Sterols: Plant sterols, often found in fortified foods and supplements, can help lower LDL cholesterol levels when consumed as part of a healthy diet.
It’s important to note that cholesterol medications should be taken as prescribed by your healthcare provider. They may have side effects or interactions with other medications, so regular follow-ups and monitoring are essential.
Remember, managing plaque buildup requires a comprehensive approach combining lifestyle changes and appropriate medications. By making these positive changes, you can effectively reduce plaque, lower cholesterol levels, and improve your overall cardiovascular health.
Conclusion
Plaque buildup and cholesterol-like plaque formation are major contributors to heart disease and cardiovascular events. To effectively prevent and manage these conditions, it is crucial to understand their causes, risk factors, symptoms, diagnosis, and treatment options.
One of the key steps in preventing plaque buildup is making healthy lifestyle changes. This includes adopting a heart-healthy diet that is low in saturated fats and cholesterol, engaging in regular physical exercise, and managing stress levels. These lifestyle modifications can significantly reduce the risk of plaque formation and the associated complications.
In addition to lifestyle changes, it is important to follow prescribed cholesterol medications, as they play a vital role in managing cholesterol levels and minimizing plaque accumulation. Regular monitoring of cholesterol levels through lipid panel tests is essential to assess the presence and severity of plaque buildup. Seeking medical guidance and adhering to the recommended treatment plan can help individuals maintain optimal cardiovascular health.
By prioritizing prevention and management of plaque buildup and atherosclerosis, individuals can significantly reduce their risk of heart disease and related complications. With a combination of healthy lifestyle choices, medication adherence, and regular monitoring, you can take control of your cardiovascular health and lead a heart-conscious life.

